North Shore Weekend, July 5, 2014
To sleep, perchance to dream. Aye, there’s the rub: too many of us aren’t sleeping.
According to the Institute of Medicine, as many as 70 million Americans – 22 percent of the population – suffer from insomnia, the general term for a variety of sleep disorders. The Centers for Disease Control calls it “a public health epidemic” with serious consequences for physical and mental health.
“It’s a severe problem for the individuals affected and, when you add up the costs in dollars and safety, for society as a whole,” said Dr. Thomas Freedom, director of Sleep Medicine at NorthShore University HealthSystem.
Dr. Freedom began his studies in the 1980s, when the study of sleep was considerably less sophisticated than it is today. “I found it one of the most fascinating areas of medicine, exploring brain function and addressing questions of consciousness and unconsciousness.”
Patients may suffer from a variety of disorders, said Dr. Freedom, including sleep apnea, in which breathing is interrupted during sleep; narcolepsy, which is uncontrollable daytime drowsiness; restless leg syndrome and sleep walking. Stress, depression and poor sleep habits can also impair sleep quality.
NorthShore operates two sleep labs, one in Skokie and the other in Bannockburn. Last year the practice conducted almost 4,000 sleep studies, in which patients spent at least one night sleeping over at one of the labs, to determine the nature and extent of their sleep problems.
To find out how such studies work, I volunteered to sleep over at Northshore Sleep Medicine, a private clinic in Evanston. Dr. Lisa Shives, director, went into the field after she realized how satisfying the work could be. “I liked the interdisciplinary nature of sleep medicine, since it involves neurology, psychology and much more. And as a resident and doctor, I’ve been seriously sleep-deprived myself, so I can empathize with my patients.”
Dr. Shives started the clinic in 2007 and has seen some 5,000 patients since then. She is leaving this summer to take an academic position at University of California in San Diego and will be succeeded as director by two physicians on her staff.
Because of a prior engagement, I reported to the clinic on the late side, after 11 p.m. My registered technician, Kristina Cornish (known as K.C.), ushered me into my private bedroom and spent the next hour administering a questionnaire, explaining the procedures and connecting my electrodes. There were wires connected to my scalp, arms, chest, abdomen, finger, legs – even in my nostrils, to monitor my breathing and oxygen levels. I had so many on my head that KC supplied me with a face net to keep everything in place.
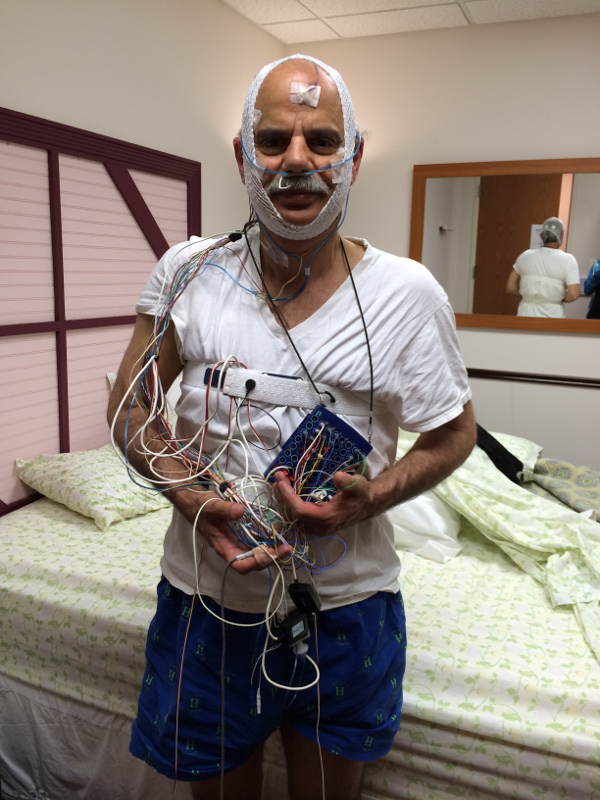
After an hour reading, I turned out the light and, surprisingly, fell asleep right away. All the wires attached to me were loose and flexible and not especially uncomfortable. The fact that KC was in a nearby room monitoring my every sigh and snore didn’t bother me, since I couldn’t see or hear her.
When I woke up in the middle of the night, I called for KC, as instructed, and she came in and disconnected me so I could use the adjacent bathroom. She awakened me at 6:45 and within 20 minutes I was heading home. Several days later I got the report: everything was normal.
Most patients aren’t so fortunate. For sleep apnea, the most common sleep disorder, patients may need a CPAP or similar device, which involves a mask connected to a machine that provides a patient with continuous positive airway pressure at night to help keep airways open. Dr. Shives said such devices are almost always effective if used as directed.
Other sleep disorders may require medication, behavioral therapy, improved sleep hygiene or other remedy.
“It’s a wonderful, feel-good specialty,” said Dr. Shives. “People usually aren’t desperately sick, and we can make them feel so much better.”




+ There are no comments
Add yours